Ozempic and other GLP-1 Agonists Cause Depression and a Significant Increased Suicide Rates in its Users
- At April 17, 2026
- By Katherine
- In Aging-In-Place, Articles, News
 0
0
Researchers have found that users of the weight loss drugs, called GLP – Agonists, but especialy Ozempic, have rapidly declining mental health, published in the journal Innovative Clinical Neuroscience, a surprising and unexpected effect. This shows that these drugs have not been studied adequately before coming to market. So why did FDA allow this? It shows iresponsibiity and negligence, in my opinion.
This issue must be addressed before severe depression occurs, as it increased significantly suicide risk, and showing a high suicide risk rate equivalent to around 15%, according to psychiatry investigations.
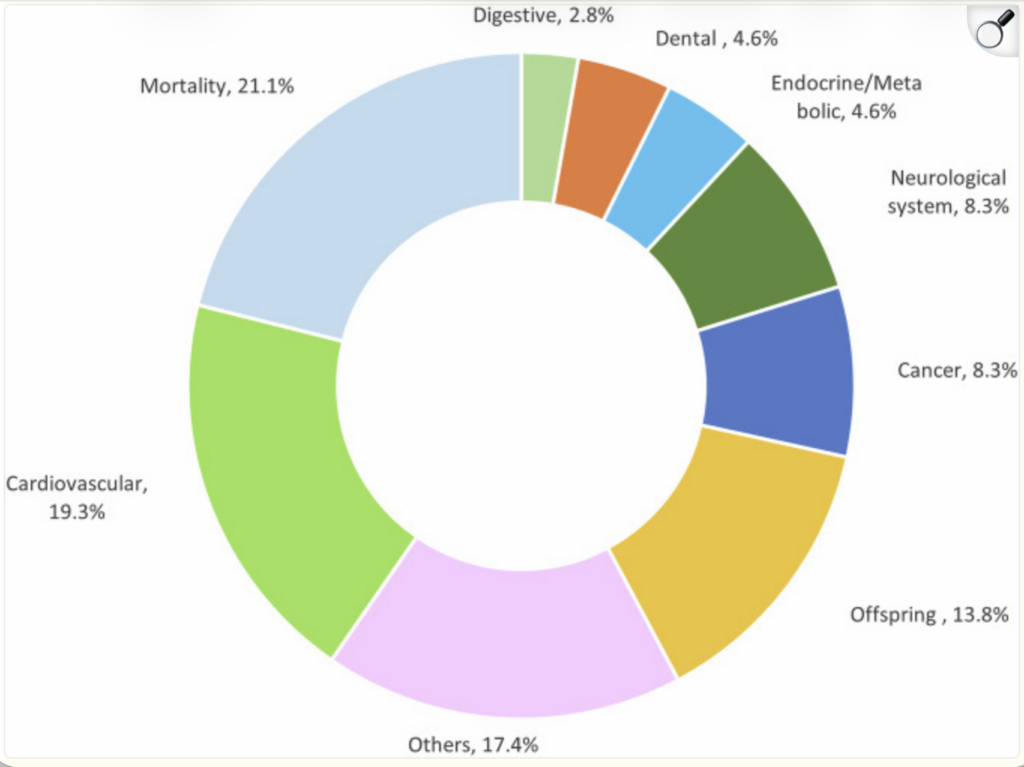
Depression has a significant impact on health outcomes, too, primarily mortality and cardiovascular outcomes. Depression affects approximately 5% of adults worldwide, as the World Health Organization estimates, and it stands as the fourth most common disease globally.
Recently, increasing number of studies have shown that depression can lead to a significantly high suicide risk, and various health outcomes, such as cardiovascular disease, atrial fibrillation, heart failure, coronary artery disease, myocardial infarction, stroke, and hypertension and impacts life quality and longevity. Depression also increases the risk of mortality, including cardiovascular mortality and all-cause mortality in cancer.
According to the Journal Transl Psychiatry, assessments of depression based on self-reports and clinical interviews show a positive correlation between depression and the risk of all-cause mortality in diabetic patients. Furthermore, depression elevated the risk of death for individuals with coronary artery disease and chronic kidney disease.
Depression not only increased the all-cause mortality among cancer patients, but also heightened the all-cause mortality rates by 34 and 30% in lung cancer and breast cancer patients with depression, respectively.
Furthermore, patients with bladder cancer, colorectal cancer, hematological cancers, kidney cancer, and prostate cancer who also have depression experience increases in cancer-specific mortality by assessments of depression based on self-reports and clinical interviews, show a positive correlation between depression and the risk of all-cause mortality in diabetic patients.
And depression elevated the risk of death for individuals with coronary artery disease and chronic kidney disease (CKD). Depression not only increased the all-cause mortality among cancer patients (RR = 1.24), but also heightened the all-cause mortality rates by 34 and 30% in lung cancer and breast cancer patients with depression, respectively. Not only do these rates increase, patients with bladder cancer, colorectal cancer, hematological cancers, kidney cancer, and prostate cancer who also have depression experience increases in cancer-specific mortality by and 87%, respectively.
Patients with peripheral artery disease, stroke, myocardial infarction, and heart failure who had depression showed an increased all-cause mortality. Among patients with coronary heart disease, depression significantly raises mortality risk, for short-term (within 2 years) mortality and for long-term mortality. Compared to patients without depression, those undergoing coronary artery bypass grafting, or percutaneous coronary intervention, with depression experienced a 41 and 76% increase in all-cause mortality.
Depression had a significant impact on the overall survival of patients undergoing hematopoietic stem cell transplantation, with a hazard ratio of 1.06. Patients with peripheral artery disease, stroke, myocardial infarction, and heart failure, who had depression, showed an increased all-cause mortality. Among patients with coronary heart disease, depression significantly raises mortality risk, short-term (within 2 years) mortality and long-term mortality.
Compared to patients without depression, those undergoing coronary artery bypass grafting or percutaneous coronary intervention, with depression experienced a 41 and 76% increase in all-cause mortality. Depression had a significant impact on the overall survival of patients undergoing hematopoietic stem cell transplantation, with a hazard ratio of 1.06.









